Striving for 5: Limit Diabetic Wounds & Their Severity


Ready or not, we are closing down the month of November and arriving at the flurry of holidays and activities! November also brings the recognition of National Diabetes Awareness Month. Ready or not, more than 30 million Americans have diabetes (9.4% of the population). These numbers from the CDC include approximately 7 million people who have diabetes but have not yet been diagnosed with it. The even more daunting numbers estimate that by the year 2050, predictions are that 1 in 3 Americans will have diabetes. And ready or not, at diagnosis, 50% of diabetics are already experiencing complications related to their disease. Many of these complications contribute to the development of wounds and interference with their healing.
If you find yourself, or a loved one, in this segment of the population, what can you do to minimize some of the effects of this disease?
While all wounds that occur on diabetics are not necessarily directly caused by diabetes (i.e. trauma, surgery, or bug bites just to name a few), they may have issues healing because of the disease. It is well known that diabetes affects ALL areas of the body including circulation, eyesight, digestion, sensation, and movement. Let’s focus on some things that you can control that can go a long way for both prevention and healing.
Strive for addressing these five areas to limit the power that diabetes has on the incidence and severity of wounds. Four out of five will be covered this month:
SUGAR (or more accurately BLOOD GLUCOSE):
It’s very important to keep blood glucose under control for healing. High glucose impairs all stages of wound healing, from responding to infection, delivering oxygen to the wound, and repairing the injured tissue. Specifically, research shows that levels under 200mg/dL support healing. If blood glucose is higher than 200, then there is much more probability of poorly healing and non-healing wounds. Remember, sugar is contained in many foods that are usually deemed healthy, such as fruit and “good carbs”. Work with your health care team to get your daily glucose under control. It will help all of your systems!
SMOKING (as in, please stop!)
As we have known for years, smoking is quite detrimental to one’s overall health. Specific to wound healing, smoking has very similar effects to high blood glucose. While the high sugars wreak havoc over a long period of time, smoking wreaks havoc (and reeks J) with EACH cigarette. One cigarette will constrict flow of blood, will decrease oxygen carried to the wound, will impair the body’s ability to fight infection, and will interrupt the repair and strengthening stages of wound healing. Smoking is double trouble with diabetes: evidence shows it may make your body more resistant to insulin, resulting in higher sugars.
Photo by http://www.health.com/smoking
STAYING SEDENTARY
Have you heard the saying: “Sitting is the new smoking”? Dr. James Levine coined this phrase a few years ago in regards to how our sedentary lifestyle “is more dangerous than smoking…that we are sitting ourselves to death”. Our wonderful technology has made much of our movement unnecessary: our lives are literally at our fingertips. We can shop, watch, read, work, and communicate from our recliner. Our fitness gadgets remind us to “MOVE” after a certain amount of sitting time. Can you imagine your grandparents needing a reminder to move? Life is different now, and our bodies show it.
Lack of exercise and basic lack of movement contributes not only to heart disease, but also to generalized weakness, immobility, obesity, and depression. This is true for diabetics and non-diabetics alike. For diabetics, exercise can be an important way to lower blood sugars or to maintain glucose control. Research in both mice and man has shown that exercise speeds wound healing. Work with your physical therapist to design exercises that will not bother the wound dressing with pressure or friction but that will improve local blood flow and general cardiovascular health.
SKIN HEALTH
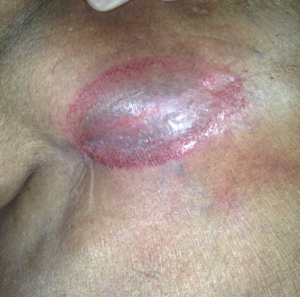
Several skin issues can plague those with diabetes. If overweight, there may be skin folds that are susceptible to increased moisture and friction, leading to a skin condition called “intertrigo”. The goal is to keep the skin folds separated from each other with textiles or absorbent materials and to allow as much airflow as possible in the area. Some medicated powder may also be helpful. This photo shows the area of the side of the chest wall, the skin fold is held open: see the line going through the middle (left to right) and how even the red area is above and below the middle line? It is a mirror image, showing how the skin is experiencing friction. This can clear up in several days if properly treated.
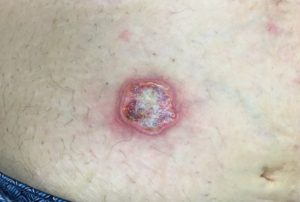
Secondly, many diabetics will develop abscesses or “boils” when glucose levels remain high. Some are diagnosed with diabetes when they develop these abscesses, go to the doctor, and have their glucose levels checked for the first time. The abscesses develop due to their body being unable to fight off bacteria and prevent a localized infection from developing. Treatment for this includes taking oral antibiotics, usually getting the abscess opened and drained, and allowing it to heal with local wound care. This is an abdominal abscess after it has opened.
The key with these skin issues is to be diligent with inspecting your skin even though it may be difficult to see everything. Develop good hygiene habits of washing and drying all areas thoroughly, feeling and looking for areas of different skin, whether it’s harder, rougher, higher, or more tender than usual. Bring any concerns to your doctor. If you cannot see well – or feel with your fingers well – find someone you trust to help you with this. It may be humbling, but it may save you some serious complications.
STEPPING SAFELY
Our fifth area requires its own section to fully discuss how to care for your diabetic feet. Stay tuned next month!

This blog post was written by Robin Carlson, PT CWS
What is PT CWS? Physical Therapist and Certified Wound Specialist